Thickened, swollen limbs are unfortunately quite common in horses. A horse’s very nature and his environment contribute to scrapes, bruises, cuts, punctures and all sorts of miscellaneous trauma to legs. Usually, this type of trauma is minimal and the swelling resolves easily. However, horses are also susceptible to cases of a more problematic type of limb swelling called cellulitis.
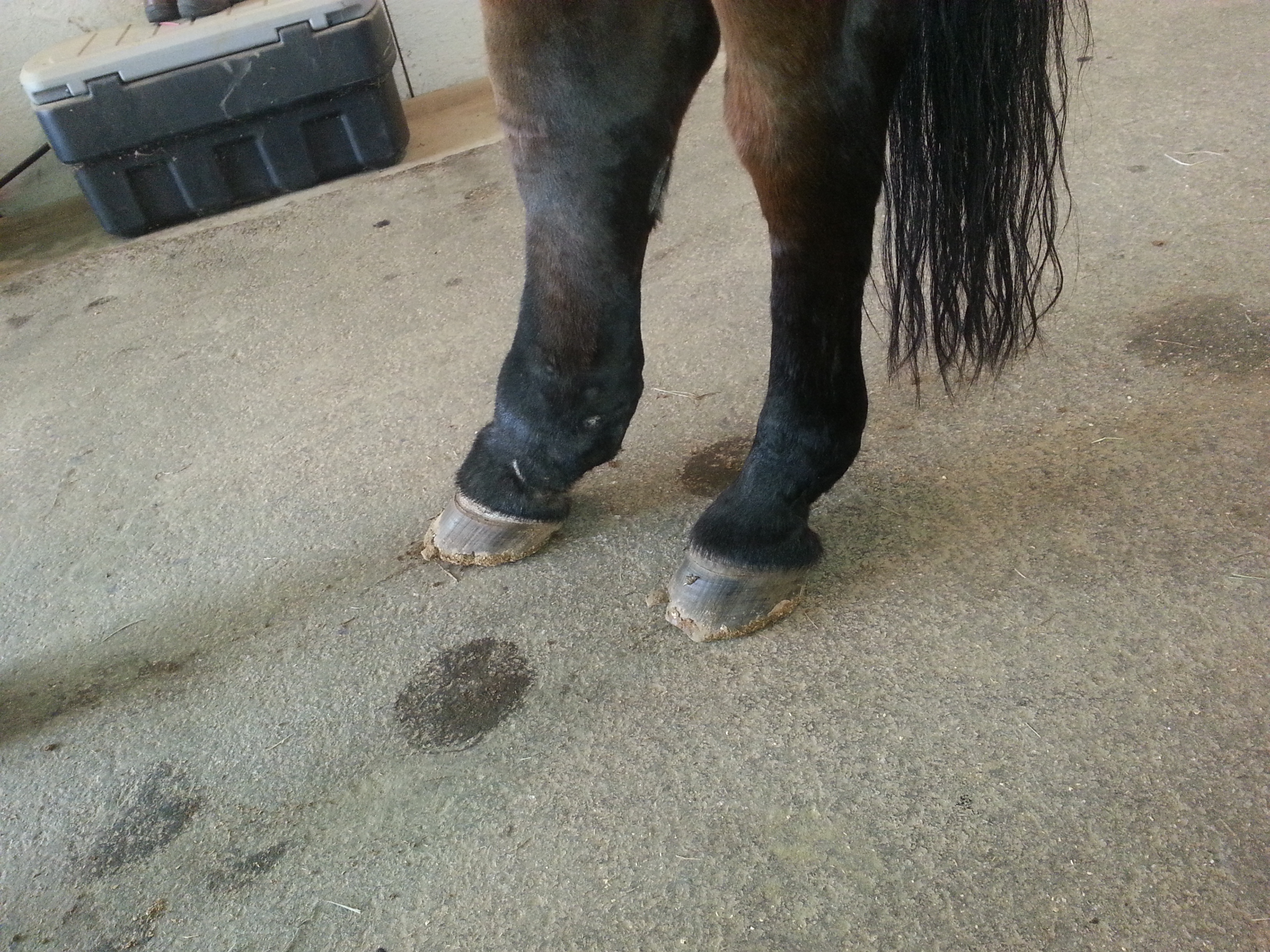
Courtesy, Kenneth L. Marcella, DVM
Cellulitis is a diffuse or widespread swelling of the skin and subcutaneous tissues (that area directly below the surface layer of the skin) caused by inflammation usually associated with bacterial infection. Some of these horses will exhibit mild signs with cool to warm swelling, minimal pain and no lameness. Other more extreme cases of cellulitis will show impressive leg swelling (two to three times the normal size), warm to hot skin that is often painful to the touch, an elevated temperature (102 to 103 degrees Fahrenheit) and notable severe lameness.
Survival rates of 55 to 89 percent have been reported for cases of equine cellulitis, with horses who have high temperatures and horses who develop laminitis in the opposite, unaffected leg having the most serious outcomes. Even if these more affected horses recover, cellulitis can recur and the prognosis for full return to function is often guarded.
This points out the variability of this condition and the wide range of severity of clinical signs. Because equine cellulitis can affect individual horses quite differently and because this disease can have potentially grave consequences, limb swelling in the horse should always be viewed seriously and treated appropriately.
The typical case of cellulitis involves a horse exhibiting a swollen leg with heat, tenderness and lameness. The peripheral area or lower part of the leg is most commonly affected and hind legs are much more likely to be involved than forelegs, though there is no reported reason for this observation. Usually only one leg is involved.
Many horses will exhibit cold, non-painful swelling, often in both hind limbs and possibly all four legs, after standing in the stall overnight. This “stocking up” type of swelling will at least partially resolve with turnout or exercise and is easily differentiated from the more serious, generally single-leg swelling seen with cellulitis. Owners have discovered cellulitis cases in horses who were out at pasture and in horses who had been stalled.
Despite exhaustive searching, almost 50 percent of cellulitis cases will not have discernible signs of trauma and can leave both owners and veterinarians frustrated as to their cause. This is called primary cellulitis, where there is nothing to indicate how or where the bacteria entered the leg. This does not mean that some type of trauma has not occurred, only that the disruption of the skin is so small that it is undetectable.
The severe limb swelling in cellulitis cases often contributes to the difficulty in finding a point source for infection. These cases are much more difficult because other causes of hot, tender leg swelling and lameness must be considered and eliminated. Fractures, severe tendon/ligament damage, vascular inflammation and joint problems must all be tested for and ruled out prior to arriving at a diagnosis of cellulitis.
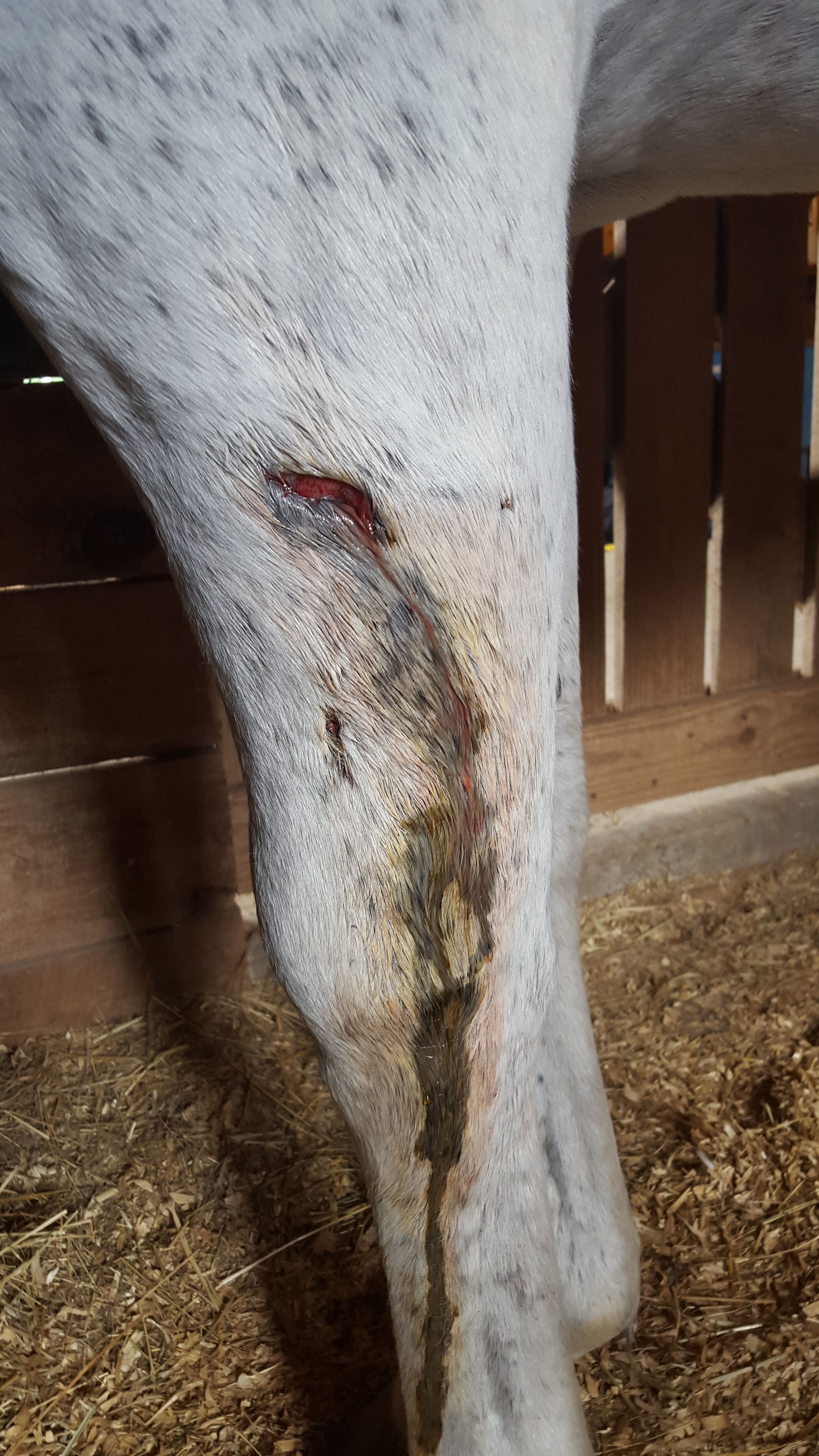
Courtesy, Kenneth L. Marcella, DVM
Secondary cellulitis occurs when bacteria enter the leg through a joint injection, surgical procedure, cut, puncture, bruise or other known traumatic source. These cases are usually more straightforward and because owners or caretakers tend to notice a cut or puncture, veterinary attention is more commonly sought for these horses at an early stage. Trauma causes a break in the protective skin surface and bacteria gain entry into the tissues of the leg. These bacteria release toxins that cause widespread inflammation and damage to the blood vessels and lymphatic channels in the lower leg.
This toxin response causes increased fluid leakage from damaged vessels and decreased fluid resorption from damaged lymphatic channels. The end result is fluid build-up, called edema, leading to the more generalized condition—cellulitis. While most cases are single events, some horses are prone to recurrence and repeated swelling. These cycles of damage to vessels and lymphatic structures can lead to permanent thickening of the leg and decreased performance.
The most common types of bacteria isolated from equine cellulitis cases are those bacteria that populate the skin surface. Staphylococcus and streptococcus are typically cultured and, therefore, antibacterial treatment for cellulitis is generally directed at these specific types of bacteria.
Severe cases may benefit from intravenous regional limb perfusion with antibiotics, which substantially increases the concentration of systemic antibiotics in the area of infection. Anti-inflammatory drugs are also commonly used along with antibiotics to treat cellulitis. Flunixin meglumine (Banamine), phenylbutazolidin and dexamethazone are routinely administered. Topical combinations of DMSO, nonsteroidal anti-inflammatories and corticosteroids have also been utilized.
The relatively recent arrival of diclofenac cream (Surpass/Voltaren) has provided the horse owner with one more treatment option in cellulitis cases. This potent anti-inflammatory cream can be rubbed on the skin locally, where it has the ability to penetrate and produce analgesia and to decrease swelling.
Physical therapy, such as cold hosing, hand-walking and massage, is also beneficial. The newer physiotherapy systems, such as Game Ready and others, provide cryotherapy combined with intermittent pneumatic compression. This combination of cold and pressure greatly reduces tissue swelling and can shorten the duration of cellulitis cases. Hyperbaric oxygen chambers, which increase the tissue oxygen concentration and help fight bacteria, have been utilized with positive results as well.
It is extremely important to remember to support the unaffected opposite limb. Icing, a heel pad and leg wraps, especially in the early stages when this limb is carrying significantly more weight while the tender, affected leg is rested, can help to avoid laminitis as a serious complication.
Good hygiene and lower-leg cleanliness are important in cellulitis prevention. Horses who routinely exercise in leg wraps or boots must have their legs cleaned regularly and attention should be directed at eliminating rubs and abrasions. Caution is needed when clipping lower legs as research has shown that often clipping will cause microdermal fractures and skin trauma that can provide an entryway for infectious bacteria.
Even if all precautions are taken, however, horses will still sometimes get swollen legs. Be prepared, be observant and be ready to aggressively treat cellulitis cases. Early recognition and treatment have been shown to greatly reduce the severity and positively affect your horse’s survival and athletic future.
Kenneth L. Marcella, DVM, graduated from Cornell University’s veterinary college. With a special interest in lameness and sports medicine, he has been an FEI veterinarian for more than 25 years. He travels throughout the country teaching continuing education for other veterinarians and horse owners and hosts numerous students at his practice throughout the year. He is board certified in veterinary thermography by the American Academy of Thermography and operates KLM Equine in Canton, Georgia.



