
Neurectomy, or palmar digital neurectomy, is a surgical procedure in which a portion of the nerve supply to the foot of the horse is cut or removed for the treatment of heel pain or navicular disease. The procedure was much more common before the widespread availability of MRI. This is because a proper diagnosis with the use of MRI often allows treatment to be tailored to the exact injury or disease in the complicated anatomy of the foot and heel areas of the horse. New treatments for navicular disease such as tiludronate (Tildren) or clodronate (Osphos) have also significantly helped affected horses. These two medications are classified as bisphosphonate drugs and are similar to those used for osteoporosis in women. They inhibit cells that break down bone and are approved for treating navicular disease in horses.
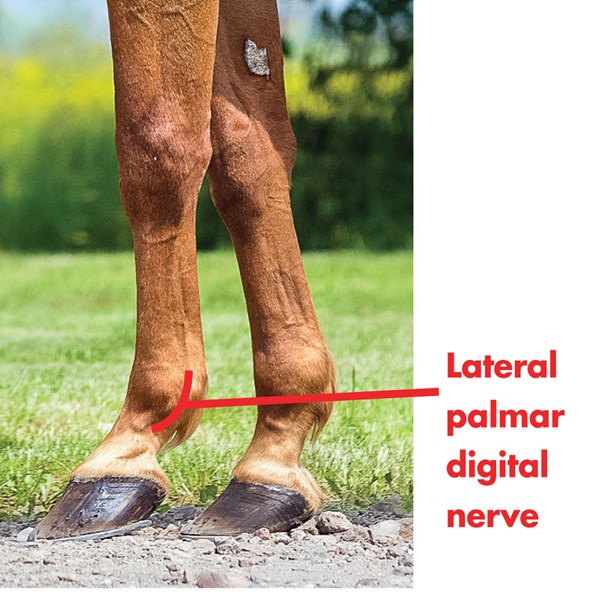
Currently, I recommend neurectomy only as a last resort when other treatment options have been performed, the horse has become refractory to other treatments and a soft-tissue injury has not been found on an MRI. Horses that are candidates for a palmar digital neurectomy should block completely to a palmar digital nerve block or a diagnostic nerve block of only the heel of the foot and have no soft tissue injury to the foot. If the lameness does not localize to the heels, then a neurectomy procedure will not be successful and the horse may remain lame.
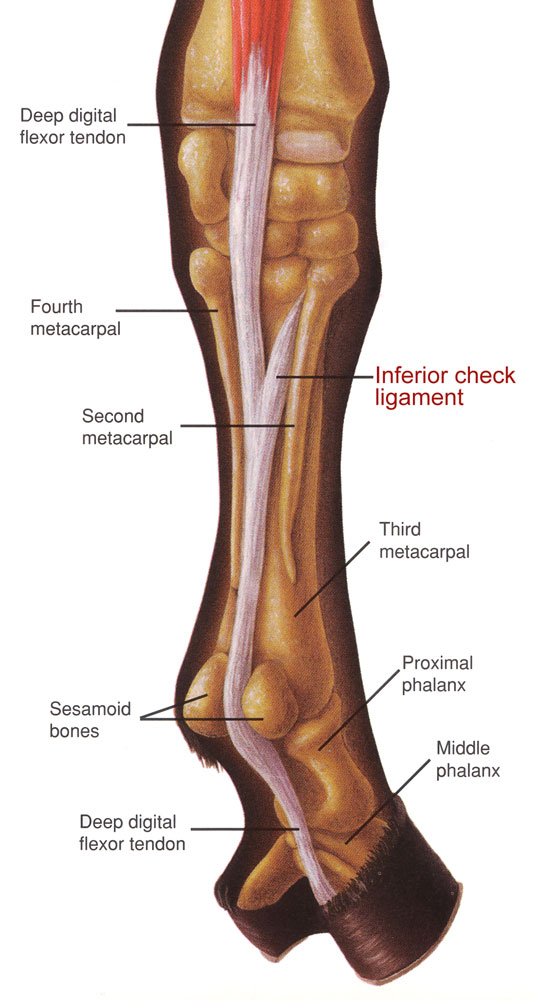
Complications of this kind of neurectomy can include formation of a painful neuroma, or ball of nerves, at the surgery site, sloughing of the foot, luxation of the coffin joint and rupture of the deep digital flexor tendon. Rupture of the deep flexor tendon or further injury to soft-tissue structures can occur if the lameness has not been properly localized to the navicular bone alone. The procedure is also not permanent as the nerves can grow back and the disease process that caused the lameness still continues. Horses that have a neurectomy procedure need to be observed carefully as they will lose sensation in the heels. So if they step on a nail, for instance, they will not feel the foreign object in the foot.
In other cases, a neurectomy of the deep branch of the lateral plantar nerve, which is closer to the area in the hock rather than the heel, is a viable option for horses with chronic suspensory disease at the origin or where the ligament attaches to the cannon bone. Pain or chronic lameness often remains even after proper treatment and rehabilitation due to enlargement of the ligament, causing a compartment-like syndrome and compression on the nerve. A very small branch of the lateral plantar nerve that supplies the suspensory origin is removed during the procedure. The main nerve supply to the foot and limb is not affected. Scientific studies have shown that neurectomy of the branch causes atrophy of the muscular component of the suspensory ligament, therefore causing a reduction in size of the ligament and improvement in nerve impingement and compartment syndrome.
Today, a neurectomy of the deep branch of the lateral plantar nerve is more commonly performed than neurectomy of the lower limb. It has a much lower complication rate than palmar digital neurectomy and presents less danger to the horse and rider as the main nerve supply to the limb is intact. If the procedure is successful and with no other underlying issues, the horse can generally return to full work. However, it is not legal to compete in FEI events after a horse has undergone a neurectomy procedure.
Laura A. Werner, DVM, MS, DACVS, joined Hagyard Equine Medical Institute in 2011 as a surgery associate in the Davidson Surgery Center and is a diplomate of the American College of Veterinary Surgeons. She specializes in lameness and equine emergency services. In addition to her experience as a surgeon, Dr. Werner is an FEI Veterinary Delegate for eventing and will soon complete her show-jumping requirement. While at Hagyard, she will be continuing her research on septic arthritis and osteomyelitis, which she began as a resident.